




























Loading. Please wait...
NEWS AND ANNOUNCEMENTS
































What are lung function tests?
Lung function tests, or breathing tests, are tests that can be done to find out how well your lungs and airways are working. Lung function tests can help in the diagnosis of respiratory (breathing) conditions, work out how severe a condition is, and help monitor the response of treatments.
Most lung function tests are straightforward and are non-invasive; however, they do require maximum effort to provide accurate results. This may be tiring and make you feel a bit breathless. but should not be painful or uncomfortable.
Preparing for your test
Please refrain from:
• Tobacco smoking / vaping/ water pipe use for at least 4hr prior
• Performing vigorous exercise for at least 4 hr prior
• Eating a heavy meal up to 1hr prior
• Consuming intoxicants / alcohol/ marijuana smoking/ caffeine drinks for at least 8 hr prior to
tests
• Wearing restrictive clothing around the chest or stomach.
A Covid RAT test must be done at home prior to arrival on the day; please bring a negative result.
Please withhold your ‘puffers/inhalers’ before testing in accordance with Medication Table
If you could not withhold these the required times because your breathing was compromised, or your doctor advised otherwise, or you simply forgot to withhold, please keep your test appointment and let the testing scientist know at the time of testing. Please note for this test the Scientist will be required to ask you age/weight/sex/height and ethnicity to adjust your lung function test.
Lung Function Tests should NOT be performed if you have had minor surgery or a concussion within 1 week of the test appointment; have had a chest infection within 2 weeks of the test appointment; have had major surgery within 4 weeks of the test appointment; have an infectious respiratory condition (eg active TB, influenza); are in late term pregnancy; have unstable vascular or cardiac conditions. If any of these apply to you, please call our rooms on 9487 8373 to reschedule or cancel as appropriate.
“Popcorn lung” is a colloquial term for a lung disease called bronchiolitis obliterans. This a serious and usually irreversible lung condition that damages the small airways in the lungs, leading to coughing, wheezing, and shortness of breath. The term originated from an incident in the early 2000s when workers in a microwave popcorn plant developed this condition after being exposed to high levels of diacetyl, a chemical used in artificial butter flavoring.
While diacetyl is most commonly associated with popcorn lung, other potential causes include:
Symptoms of popcorn lung may include:
Diagnosis typically involves a combination of medical history, physical examination, lung function tests, and imaging studies. Treatment primarily focuses on managing symptoms and may include bronchodilators and corticosteroids. However, since popcorn lung is progressive and irreversible, prevention (particularly limiting exposure to harmful chemicals) is crucial.
If you have concerns about respiratory health or exposure to specific chemicals, it’s important to consult with your GP and get a referral to be assessed by a Respiratory specialist.
The duration of a respiratory flu, commonly referred to as influenza, can vary depending on several factors, including the individual’s overall health and the specific strain of the virus. Generally, the symptoms of the flu can last anywhere from a few days to about two weeks.
Here’s a breakdown of the typical timeline:
Key characteristics of COPD include:
Chronic Bronchitis /Chronic asthma: Involves inflammation and narrowing of the airways, accompanied by excessive mucus production, leading to coughing and difficulty breathing.
Symptoms : Common symptoms include chronic cough, sputum production, wheezing, and shortness of breath, especially during physical activities. As the disease progresses, individuals may experience increasing difficulty with daily activities.
Management : While there is no cure for COPD, management strategies can help alleviate symptoms and improve quality of life. These may include smoking cessation, medications (like bronchodilators and corticosteroids), pulmonary rehabilitation, and in severe cases, oxygen therapy or surgery.
Mucus production is a natural and essential function of the respiratory system, as it helps to trap dust, allergens, and pathogens, keeping the airways moist and protected. However, excessive mucus can lead to uncomfortable symptoms, especially when conditions like sinus issues, silent reflux, or lung-related ailments such as bronchiectasis and bronchitis are present.
Chest physiotherapy is indeed a specialized area within physiotherapy that focuses on improving respiratory function and mobilizing mucus in patients with lung congestion and other respiratory conditions. At Sydney Respiratory Specialist Clinic, Ms. Vicki Hill brings extensive expertise, holding a master’s degree in chest physiotherapy and boasting over 20 years of experience. Her skills are invaluable in providing effective treatment tailored to individual needs, helping patients manage lung congestion and improve their overall respiratory health. With her guidance, patients can benefit from a range of techniques designed to enhance lung function and quality of life.
Identifying the underlying cause of lung congestion is crucial for effective treatment. A respiratory specialist can conduct thorough assessments and diagnostic tests to determine the specific issues affecting your respiratory health.
To consult a respiratory specialist or a chest physiotherapist, a referral from your general practitioner (GP) is required. This referral ensures that you receive appropriate care tailored to your needs. If you suspect you have a respiratory condition or are dealing with ongoing lung congestion, it’s a good idea to schedule an appointment with your GP for evaluation and potential referral.
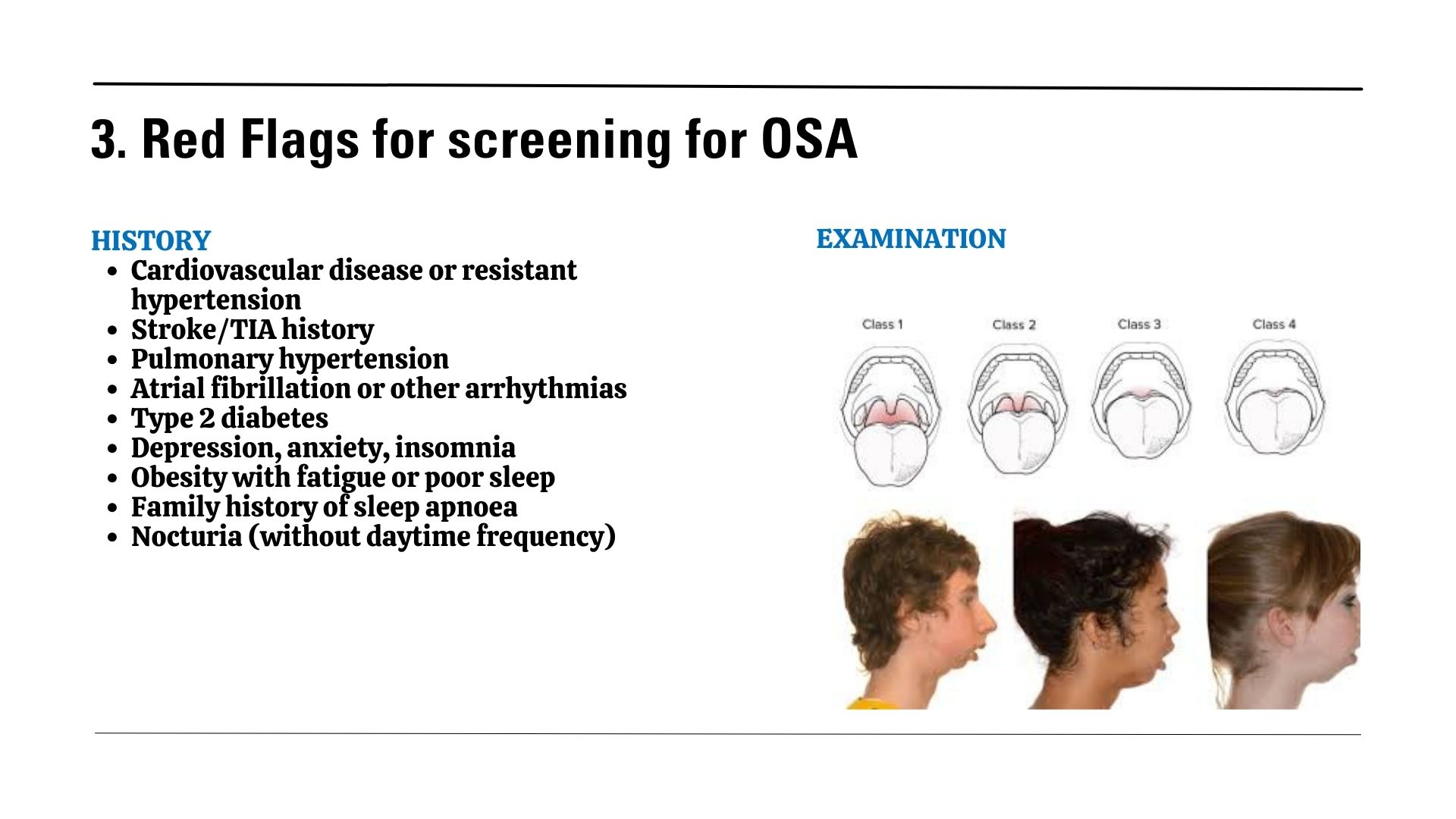
While most patients with sleep apnoea present with noticeable symptoms, such as snoring or daytime sleepiness, some individuals, especially those with severe sleep apnoea, may have dangerously low oxygen saturation levels at night without displaying any obvious signs. Women, in particular, often present with fatigue rather than classic sleep apnoea symptoms.
Sleep apnoea often goes unnoticed, earning it the title of a “silent disease.” But its impact on your health is far from quiet. Affecting millions worldwide, this common yet underdiagnosed condition disrupts your breathing while you sleep, leading to serious health risks if left untreated.
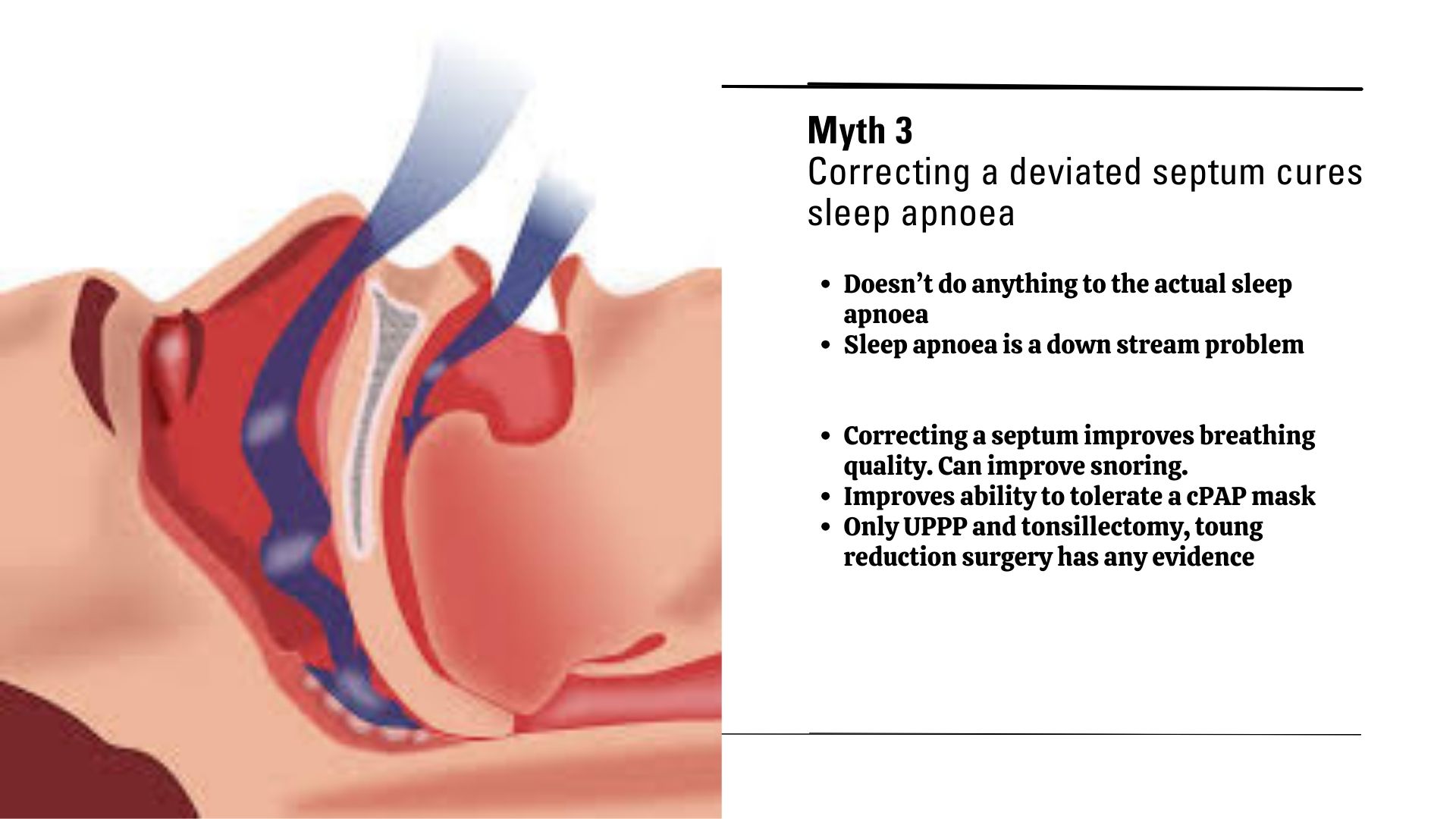
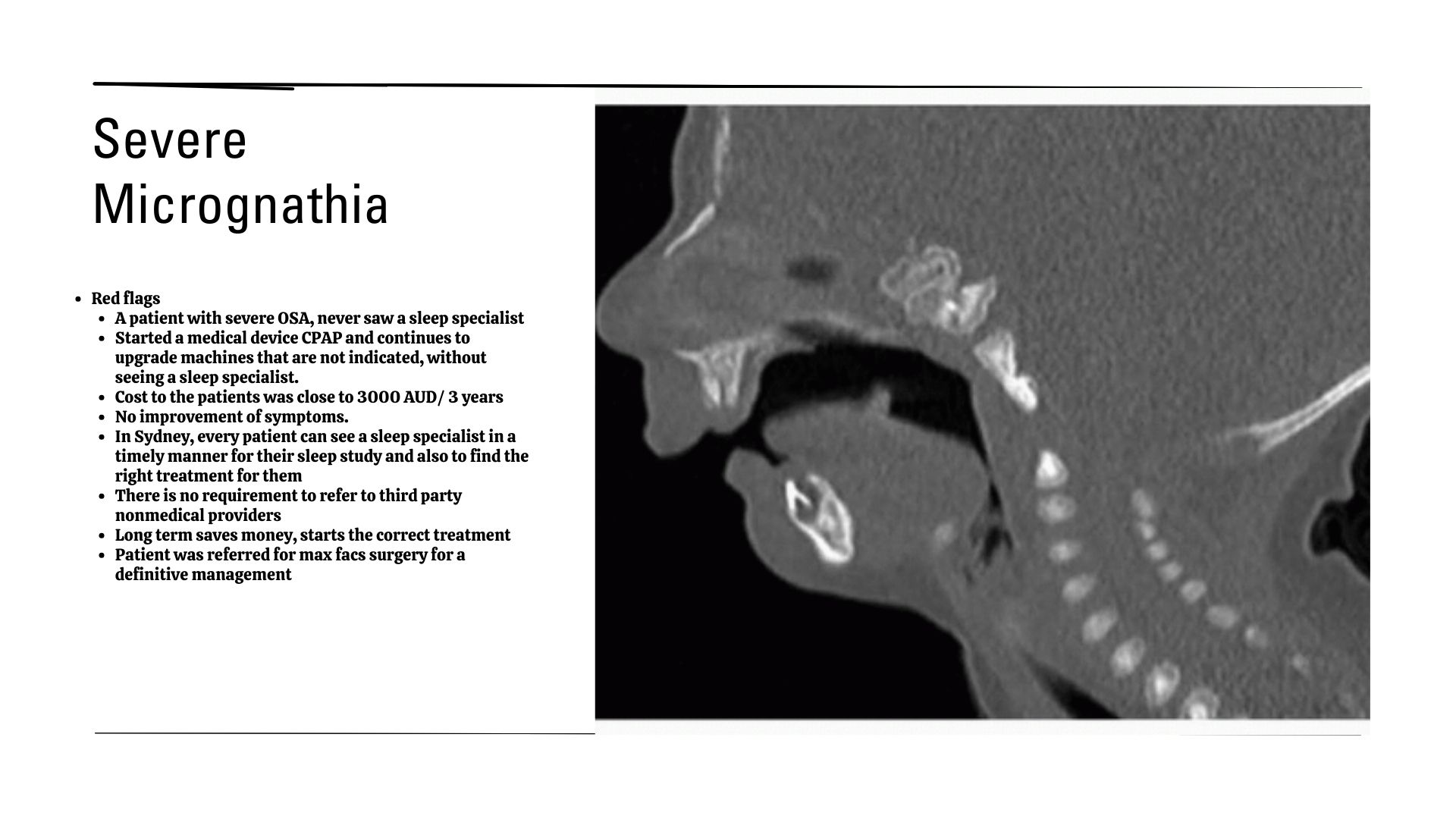
Sleep apnoea occurs when your airway becomes blocked or collapses during sleep, causing repeated pauses in breathing. These interruptions, which can last seconds or even minutes, often go unnoticed by the person affected. However, the brain is forced to wake you partially to restart breathing, fragmenting your sleep cycle.
Since you’re asleep when the pauses occur, many people remain unaware they have sleep apnoea. Common symptoms include:
If left untreated, the condition can lead to severe complications such as high blood pressure, heart disease, diabetes, and even strokes.
One of the most alarming aspects of sleep apnoea is its subtlety. Often dismissed as mere snoring or blamed on stress, it continues to affect your health in the background. Over time, untreated sleep apnoea strains your heart and limits oxygen supply to vital organs, silently compromising your well-being.
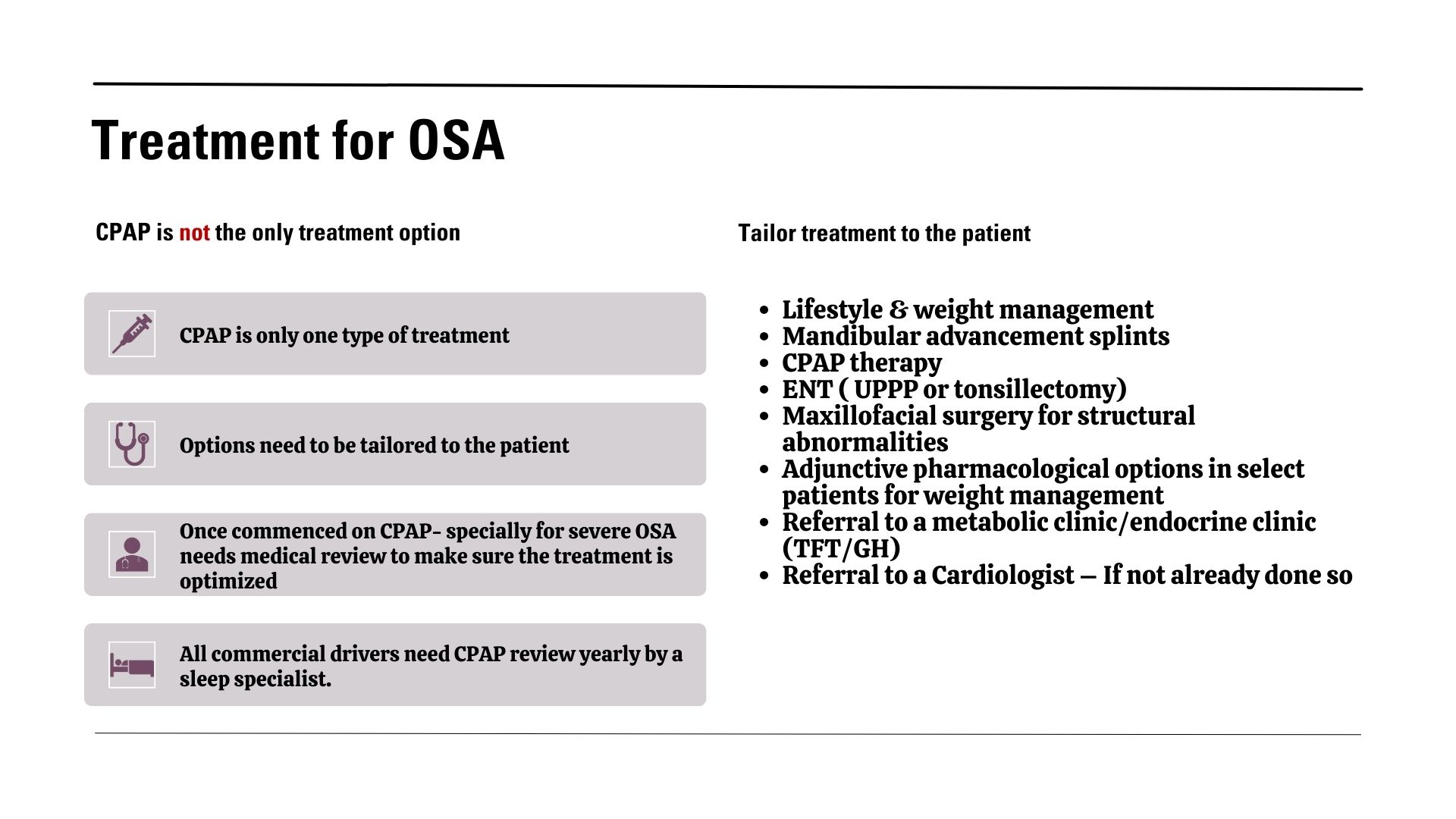
The good news? Sleep apnoea is treatable. Advances in technology have made diagnosis easier than ever, with at-home sleep studies offering a convenient alternative to traditional lab tests. Once diagnosed, treatment options include lifestyle changes, Continuous Positive Airway Pressure (CPAP) therapy, oral devices, and in some cases, surgery.
Ignoring sleep apnoea doesn’t just affect your sleep quality; it jeopardizes your long-term health. Early intervention not only restores restful sleep but also protects your overall well-being.
If you or someone you know exhibits symptoms of sleep apnoea, don’t wait. Speak to a healthcare professional and explore testing options. Your sleep—and your health—deserve attention.
Sleep apnoea may be silent, but its consequences are loud and clear. Recognize the signs, take action, and reclaim the restful sleep your body needs.
Copyright © 2024 SydneyRespiratorySpecialist. All rights reserved.